Serious mental illness (SMI) imposes devastating costs to a person’s life, impacting healthcare costs, education, work, and life expectancy. The individual economic burden of SMI is high, comparable to cancer and diabetes, and further exacerbated by the relatively young age of onset.
While there is acceptance that early intervention has lifetime benefits for people with serious mental illness, there has been little evidence to support this assumption, in part because many studies do not follow individuals for their entire life and thus cannot capture the lifetime benefits. A new study, published in the April 2019 edition of Health Affairs, uses a microsimulation model to estimate the lifetime burden of SMI for individuals diagnosed before the age of twenty-five.
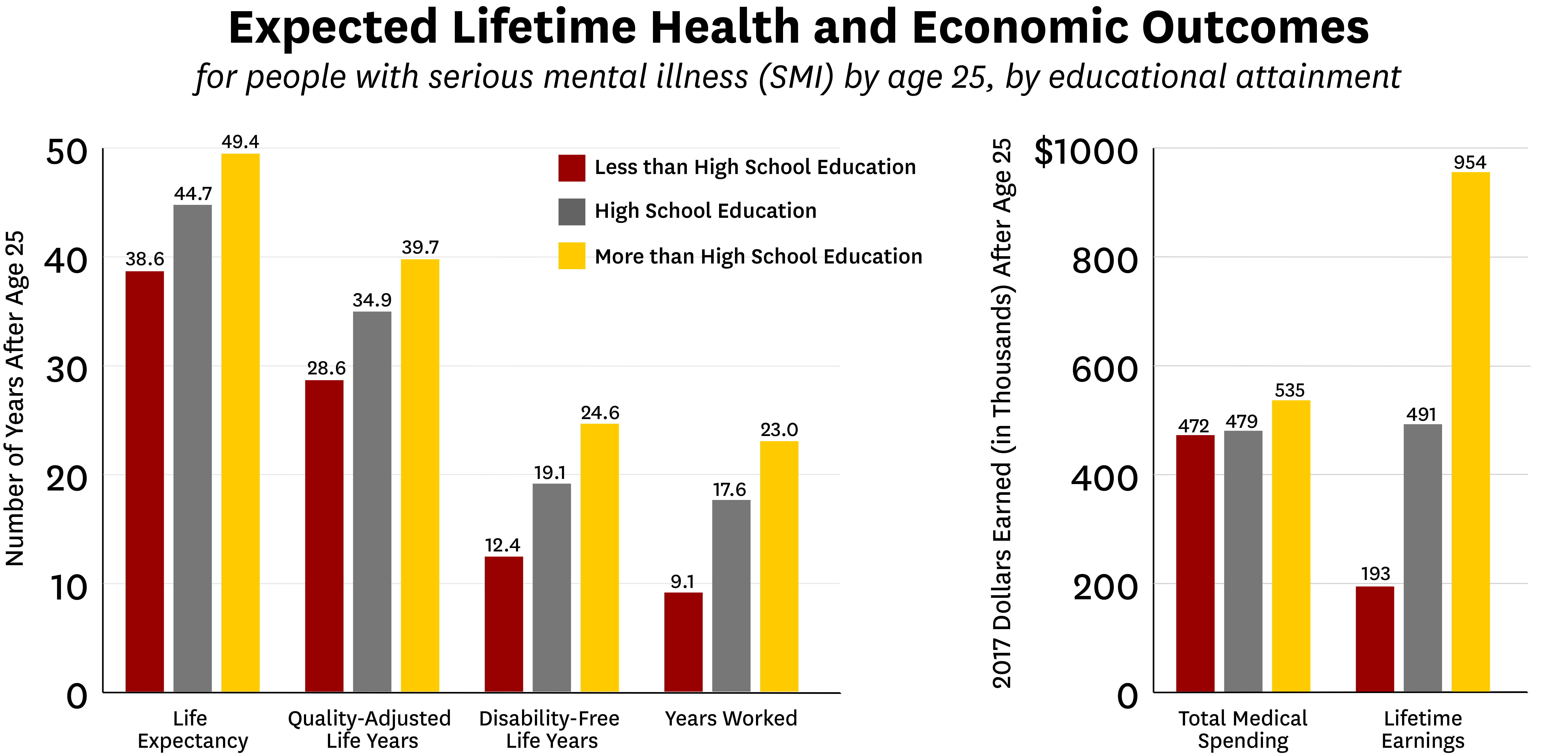
The researchers estimate the lifetime burden of SMI to be $1.85 million per patient. They also estimate that an intervention that successfully improved educational attainment for patients with SMI would result in a reduced burden of over $73,000 per patient.
Serious mental illness collectively includes psychoses, major depressive disorder, and bipolar disorder. While previous studies have shown the positive impacts of early identification, diagnosis and treatment on quality of life, they do not assess the benefits of these interventions across an individual’s life span. This study provides new data on the lifetime benefits of improving educational outcomes for people who experience SMI early in life. Using the Schaeffer Center Future Adult Model, the researchers simulated the lifetime outcomes of people with and without SMI by the age of twenty-five.
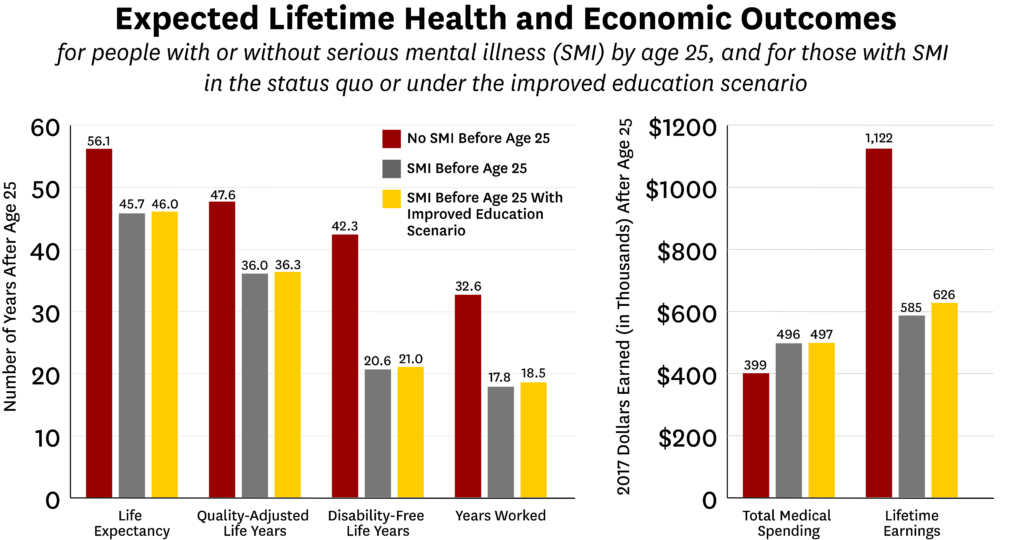
Results of the simulations show SMI significantly worsens lifetime health outcomes, raises medical costs, and reduces economic outcomes. People with SMI by age twenty-five had an average life expectancy loss of over ten years and lifetime earnings $537,000 less than those without SMI by age twenty-five.
The study results show that the economic burden of each new cohort of SMI patient experiences nearly a quarter of a trillion dollars in economic burden, and the simulated improvement in educational attainment would produce a reduction of over $8.9 billion. While such an intervention might be costly, the authors estimate a two-year educational intervention would produce a two-to-one return on investment compared to the cost of the intervention. The authors note that widely implementing the interventions necessary to spark increased educational attainment would require an investment in increasing behavioral health services.
The study was published in Health Affairs.
You must be logged in to post a comment.