Editor’s note: Posts on the Evidence Base Blog are edited for clarity, but have not been subject to a formal, peer-review process.
A few weeks ago, Los Angeles Unified School District (LAUSD) announced that it would be finally open for in person learning. To keep schools safe, as the more contagious delta variant causes another surge in Los Angeles, students attending school on the first day were required to have had a COVID-19 test in the two weeks prior to the first day. After the first day students will be tested weekly.
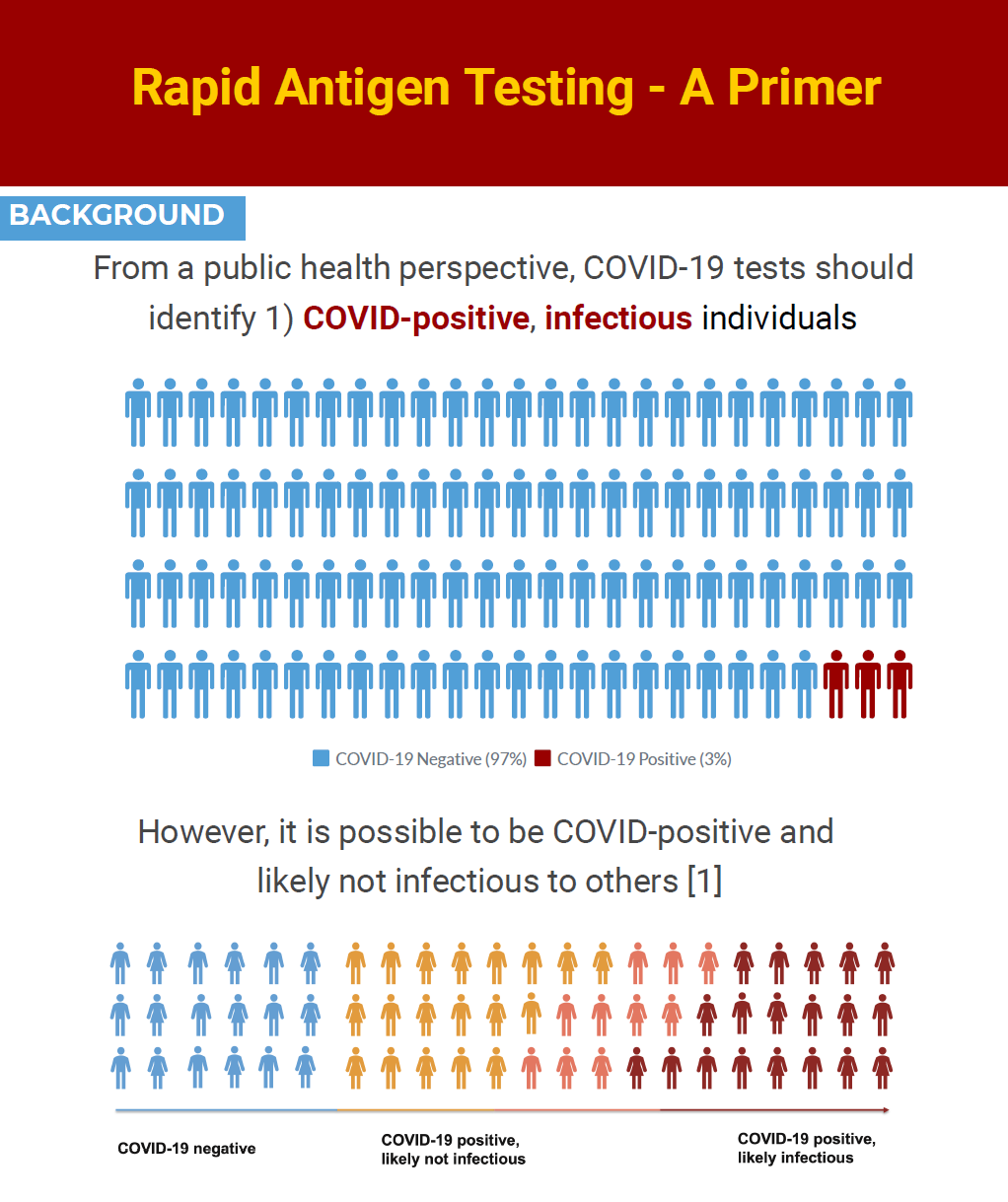
Does this strategy make sense and is it a good use of scarce resources for children’s education? To answer this, we need to understand the purpose of testing from a public health perspective.
The Role of Testing from a Public Health Perspective
There are two main goals of testing from a public health perspective. The first goal is disease surveillance or to understand disease risk. For example, the testing conducted by LAUSD showed that 8 in 1,000 children tested positive for COVID-19 in the 2 weeks prior to school opening. However, one need not test every child to understand disease risk. That can be done equally well and with a much smaller budget by testing a random sample of children. So the district could have saved millions of dollars and inconvenience for hundreds of thousands of parents and children if they had hired a couple of statisticians to design a study to conduct surveillance testing.
Sign up for Schaeffer Center news
The second goal of testing is to minimize disease risk by preventing outbreaks and disease transmission. To achieve this goal, one needs to identify students or staff who are infectious and then prevent them for attending school. Here again, the testing strategy of LAUSD is less than ideal. LAUSD has chosen to use PCR tests for testing students or staff. Even under the best of circumstances the turnaround time for a PCR test is roughly 12 hours and in practice can take much longer. This testing of students is being done during school hours. So a positive PCR test means that a child who was potentially infectious attended school. The longer the delay in getting results the longer the child will attend school. So testing did not prevent an infectious child from attending school it simply reduced the duration of attendance. For a virus as contagious as the delta variant it is unclear if just limiting the duration of attendance is enough for preventing outbreaks. Another challenge with PCR tests is false positives. That is, a PCR test result can be positive even when the child is not infectious. These false positives and associated quarantine of children and staff cause a disruption in schooling with no public health benefit.
A Better Strategy: Serial Rapid Antigen Testing in Schools
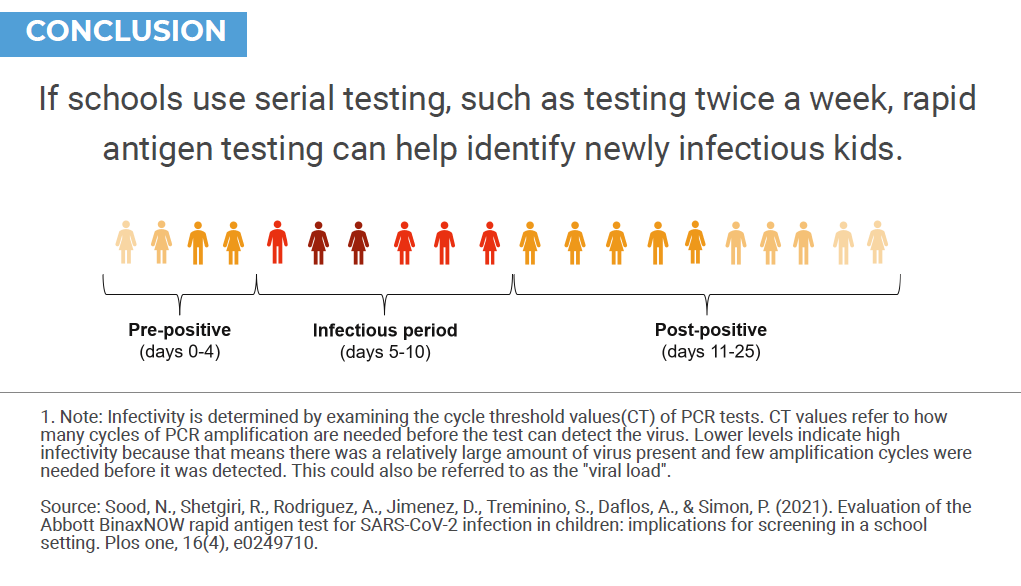
There is a better way to prevent outbreaks in schools: using rapid antigen tests to test children at least twice a week in areas with high COVID-19 risk. As noted before, the first purpose of testing is to conduct disease surveillance. If such surveillance finds low or minimal COVID-19 risk, we can verify for parents, teachers, and children that school are safe and that we don’t need to do extensive testing to prevent outbreaks. This peace of mind should not be overlooked for students, teachers, and parents. It can lead to a normal school experience generally and allow for the full range of activities children normally engage in.
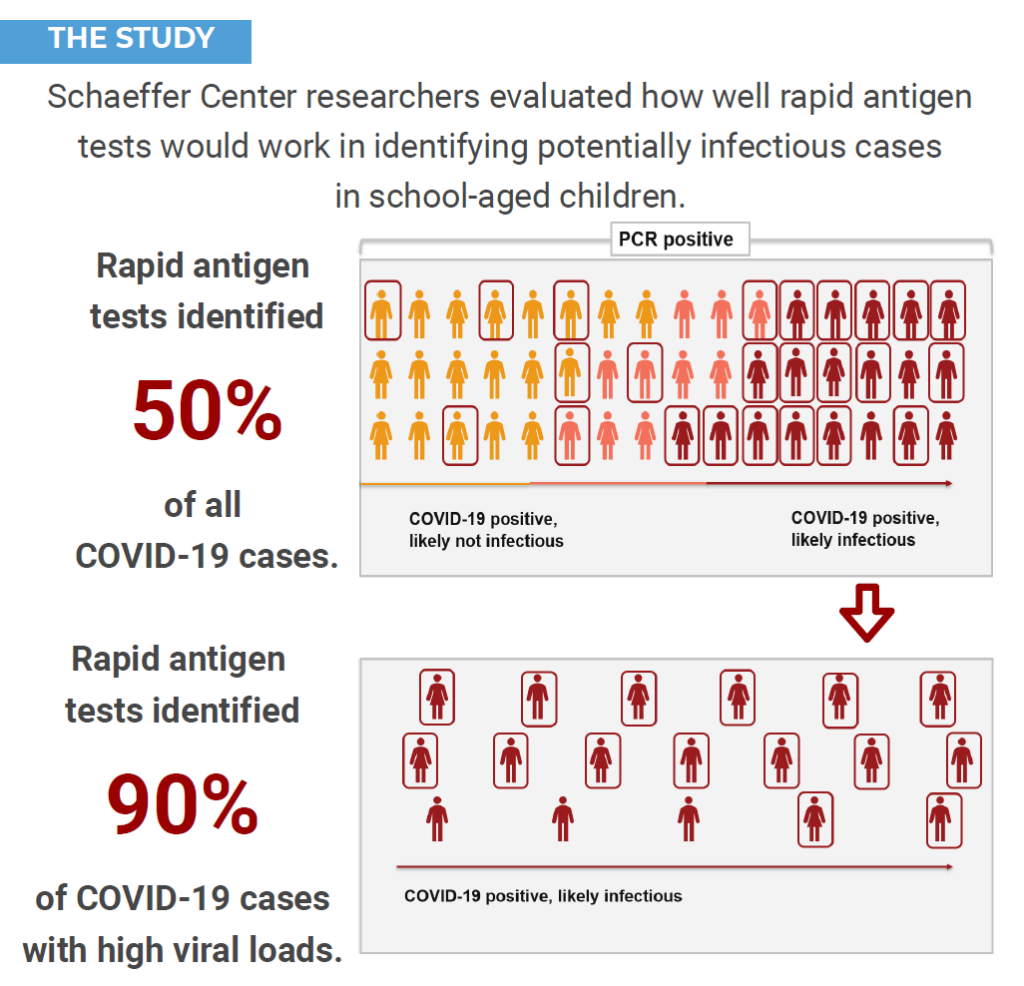
However, if surveillance testing finds evidence of high COVID-19 risks then we can use serial rapid antigen testing to prevent disease outbreaks. Serial rapid antigen testing offers several advantages over PCR tests. First, rapid antigen tests deliver results within 15 minutes. This means a child can be tested at home prior to coming to school and infectious children can be prevented from attending school. My research shows that the tests are about 90% accurate in identifying children who are asymptomatic and potentially infectious. Second, the tests are cheap and thus can be conducted more frequently. Frequent testing is key for preventing outbreaks as infectiousness can vary with time and a child who is not infectious today can be highly infectious just two days later. So testing just once a week as proposed by LAUSD is not enough, even with a perfect test, once a week testing will miss a significant fraction of infectious children. Frequent testing significantly increases the chances of catching a child during the short infectious window and research shows that more frequent testing can potentially be highly effective at preventing outbreaks.
By conducting smart surveillance testing and serial rapid antigen testing LAUSD can simultaneously save money and make schools safer.

Related Work
-
Press Release
Traditional Vaccination Playbook Doesn’t Work with COVID
-
Perspective
The High Cost of ‘Free’ Covid Testing



You must be logged in to post a comment.