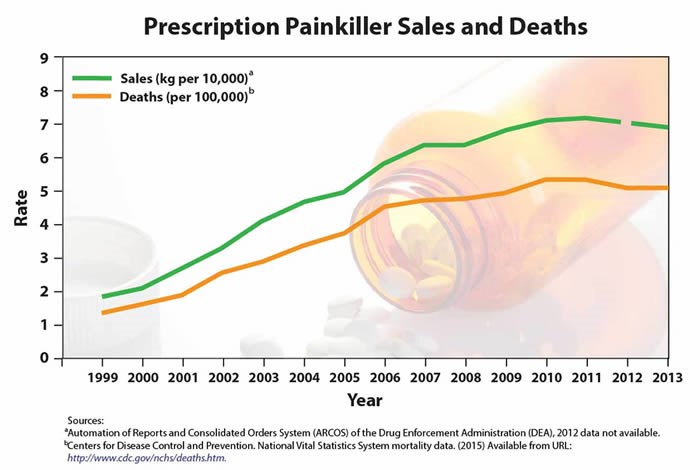
According to the CDC, in 2010 enough opioid pain relievers were sold to medicate every adult in the US with a typical dose of hydrocodone every four hours for one month. This exemplifies a more-than-tripling of opioid sales which has occurred over the past decade and is linked to negative outcomes including addiction, overdose, substance abuse treatment and increased ER visits.
A new piece of bipartisan legislation in front of the Senate Finance Committee is aimed at curbing prescription drug abuse among Medicare beneficiaries. Under the terms of the Stop Medication Abuse and Protecting Seniors Act, the co-sponsors propose a medication “lock-in” program to reduce doctor and pharmacy shopping.
Though stopping the opioid abuse epidemic is of paramount importance, there is a lack of evidence these lock-in programs are the most effective solution and may actually negatively impact vulnerable populations.
What is a medication “lock-in” program?
A medication lock-in program limits beneficiaries who are deemed to be abusing prescription drugs to only obtaining these controlled substances from one physician and one pharmacy. Through limiting prescriptions for opioids and other pain killers to one physician and one pharmacy the ability for a beneficiary to shop around- and thereby fill multiple prescriptions of the same prescription pain killer- is reduced. This policy is common in both Medicaid and in private insurance arrangements, but is not allowed under the terms of the Medicare program.
While as many as 46 state Medicaid programs have implemented such lock-in programs, there is a dearth of evidence on their effectiveness in reducing or reversing prescription drug abuse. Furthermore, most assessments have focused on the ability of these programs to save money, rather than address the underlying problem of substance abuse.
What do we know about prescription drug abuse in Medicare?
A basic problem in gauging whether such a law might impact prescription drug abuse in the Medicare population is our lack of research on not just controlled substance abuse, but also opioid use among Medicare beneficiaries.
When trends in opioid use are broken down by state, the percentage of prescriptions filled by Medicare Part D beneficiaries varies considerably. According to a recent MedPAC report, 32 percent of Medicare Part D beneficiaries filled a prescription opioid in 2011: by state, this statistic ranged from 44 percent of beneficiaries in Alabama to only 20 percent in Hawaii.
A study by my colleagues at the Schaeffer Center found that among all opioid users in 2010, about 12 percent received opioid prescriptions from four or more physicians.
While these and a few other studies (see GAO study, CMS study, Dartmouth study) provide some perspective on the scope of utilization or misuse they focus on isolated outcomes or single-year snapshots. Without better evidence on how these controlled substances are being utilized by Medicare beneficiaries, it is impossible to judge whether a lock-in program would be successful.
What are the possible negative consequences of medication lock-in programs?
It is also possible that medication lock-in programs could have unintended consequences for individuals whose healthcare requires these prescriptions.
For example, if the lock-in program honed in on beneficiaries (as is common in Medicaid programs) with frequent prescriptions, multiple prescribers, and multiple pharmacies, we have little sense of how common that might be. In preliminary research, I find that anywhere between 2 and 16 percent of opioid users could fit such a definition. Without careful consideration of the terms, it is likely that many beneficiaries who are not abusing controlled substances could fall within the scope of such a program—putting their access to important medications in jeopardy. Further, existing disparities in access to controlled substances could be exacerbated if patients who must shop around to get necessary care are further restricted.
While tackling the opioid epidemic head on is an important priority for Congress, I would urge them to assess the effectiveness and impact of similar programs in Medicaid and private insurance before implementing them in Medicare. I would also caution them to think carefully about how they define prescription drug abuse as casting too wide a net could jeopardize vulnerable beneficiaries.
But, before anyone can propose effective solutions to this problem, we need to accurately quantify prescription opioid use and abuse in Medicare and continue to analyze the trends in opioid prescriptions as well as the characteristics of utilization.